CARDIOVASCULAR DISEASE
Located at the left side of mediastinum
A. LAYERS
Epicardium - covers the outer surface of the heart
Myocardium - middle layers; contracting muscle
Endocardium - innermost layer; lines inner chamber and heart valves
B. PERICARDIUM - encases and protects the heart from trauma and infection
Parietal Pericardium - Tough fibrous membrane that attach to the sternum, thoracic vertebrae and diaphragm
Visceral Pericardium - Thin membrane that attach to the heart
Pericardial Space - In between: holds 5-20 ml 0f fluid which lubricates the pericardial surfaces
C. HEART CHAMBERS
Right Atrium - receives deoxygenated blood from the body via SVC and IVC
Right Ventricle - receives blood from the RA and pumps it to the lungs via Pulmonary Artery
Left Atrium - Receives oxygenated blood from the lungs via the 4 pulmonary veins
Left Ventricle - largest and most muscular chamber and receives oxygenated blood from the LA and pumps blood into the systemic circulation via aorta
D. HEART VALVES
Atrio-Ventricular Valves - lies between the atria and the ventricles Closed at the beginning of ventricular contraction and prevents blood from flowing back to the atria, Opens when ventricles relax
Semilunar Valves - Opens when ventricles contact and prevent blood from flowing back into ventricles, Closed when ventricles relax
Bicuspid or Mitral Valve - located at the left side of the heart
Tricuspid Valve - located at right side of the heart
Pulmonic Valve - Between RV and Pulmonary Artery
Aortic Semilunar Valve - Between LV and Aorta
E. ELECTRICAL CONDUCTIVITY OF THE HEART
Sinoatrial Node (SA node) - Pacemaker of the Heart; initiates each heart beat
Located at junction of SVC and RA
Generates electrical impulse at 60-100 times/ min
Atrioventricular Node (AV node) - Located at the lower aspect of the atrial septum
Receives electrical impulse from the SA node
Bundle of HIS (AV Bundle) - Fuses with AV node to form another pacemaker site
Branches into the left and right Bundle Branch and terminates into Purkinjie Fibers
If SA node fails it can initiate and sustain HR of 40-60bpm
Purkinjie Fibers - Spread waves of depolarization through ventricles
F. CORONARY ARTERIES - Supply the myocardium with blood
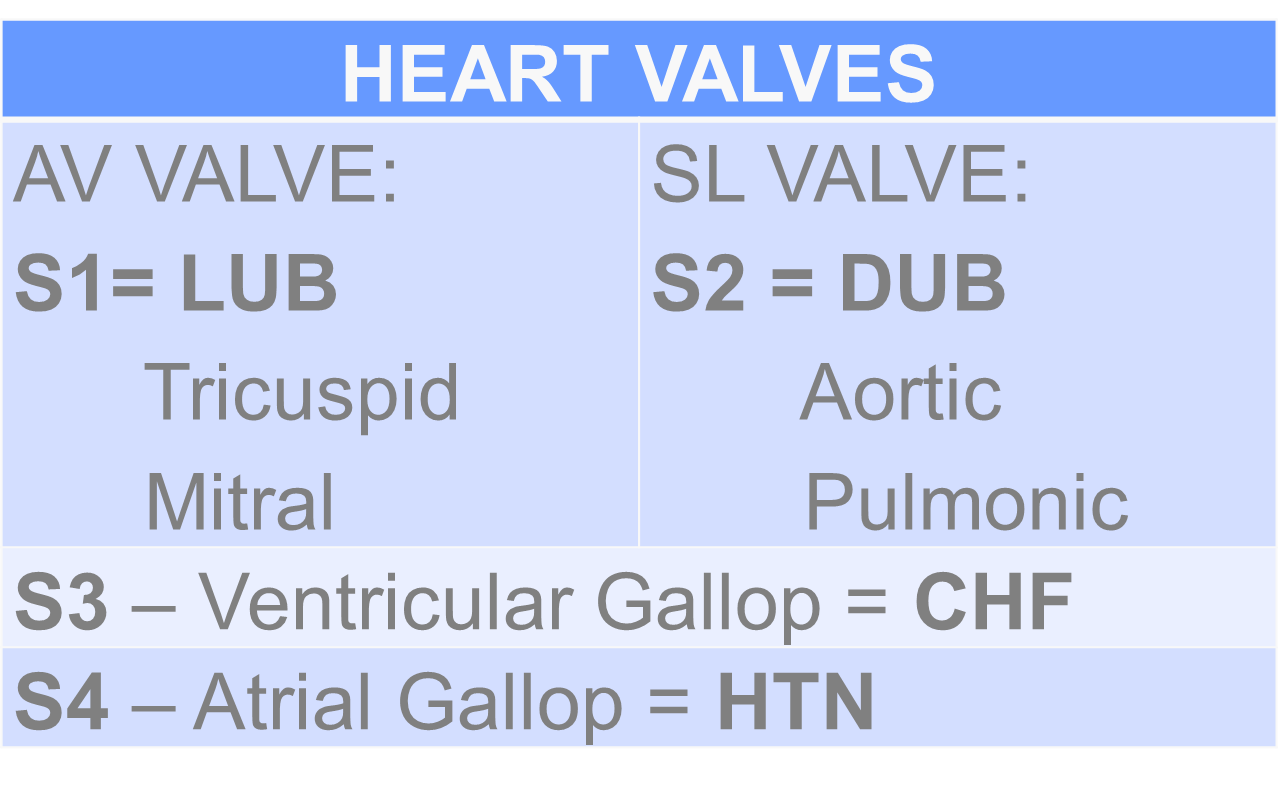
G. HEART SOUNDS
S11st heart sound - heard when AV valve closed
S2 2nd heart sound - heard when semilunar valve closed
S3 3rd heart sound - CHF
S4 4rth heart sound - HTN
I. ATHEROSCLEROSIS
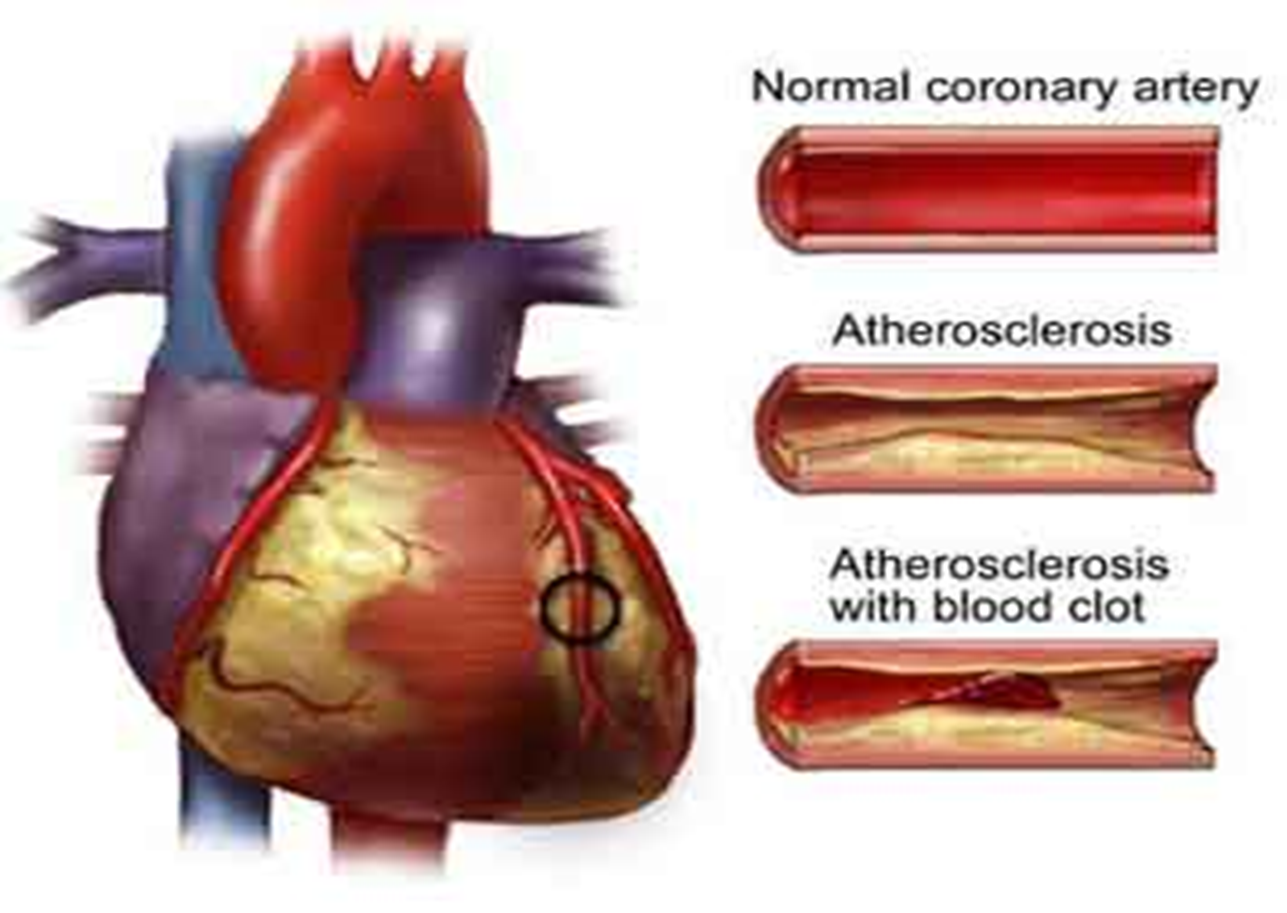
Diagnostic Tests
1. STRESS TEST = non-invasive, studies heart during activity and evaluates coronary artery disease
Treadmill = Most common
Radionuclide = Injected for perfusion and imaging
If the patient cannot tolerates stress test – persantine (Diphyridamole)
After the procedure avoid Hot Shower
2. ECG = Records electrical activity
1st test to MI patients
3. LABORATORY
A. Cardiac Enzymes
CK-MB = most definitive of cardiac damage, it rises within 4-6 hours
LDH = Rises within 1-2 days
if LDH 1 is higher than LDH 2 = MI
Troponin I = Rises within 3 hours
Myoglobin = Rises after 1 hour
SGOT/AST
B. CBC
RBC rises due to inadequate oxygenation
WBC rises due to necrotic tissue
HCT decreases due to decreased vascular flow
4. NUCLEAR CARDIOLOGY = radionuclide and scanning
Technitium Pyrophosphate Scanning
Thallium Imaging
Multigated Cardiac Blood Pool Imaging
Hot-spots viable tissue of the Heart
Cold-spots-necrotic tissue of the heart
5. CARDIAC CATHETERIZATION
Best Test for Cardiac Pathology, determines the patency of the artery (Femoral or Brachial)
NURSING CONSIDERATIONS
Informed Consent
Assess for allergy to seafood, iodine and dyes
NPO 6-8 and liquids 4
Fluttery feeling- when the catheter passes to the heart
Flushed warm feeling-when the dye is injected
Desire to cough and palpitation- due to irritability
Check most distal pulses
Apply sandbag- 4 hours check for bleeding
Keep extremities extended
Check for bleeding- 6 hours apply ice
Encourage Oral Fluid Intake- to excrete dye
NURSING INTERVENTIONS
1. COMFORT THE PATIENT
Drug of Choice
Nitroglycerine - Vasodilator: Angina Pectoris
Complication: O. HTN, Dizziness, Headache
Aspirin with NTG to prevent Headache
Given 3x with an interval of 5 minutes
Expires within 6 months
Apply to non-hairy part except forehead to prevent syncope
Morphine Sulfate: Myocardial Infarction
Narcotic, Depressant, Analgesic
Antidote: Narcan (Naloxone)
if effective: causes hyperventilation
Complete Bed Rest
Oxygen Inhalation
Work Quietly and Systematically
2. HEMODYNAMIC STABILITY
Monitor Vital Signs
Pulse Rate: Monitors skip beats it can lead to arrhythmia
DOC is Xylocaine (Lidocaine)
H - Hypokalemia
- Hypocalcemia
- Hypometabolic State
- Hypoxia
A - Acidosis
T – Toxic Agents (Digoxin)- Cardiac Glycoside
E – Exercise
CARDIOGENIC SHOCK
If Blood Pressure goes DOWN
Narrowing of Pulse Pressure
Oliguria ≤ 400 ml
Altered Level of Consciousness
NURSING INTERVENTIONS
1. Adrenergic Agonist – Increases Myocardial Contraction
Dopamine (Intropin)
Dobutamine (Dobutrex)
Titrate according to patients Blood Pressure
Epinephrine (Adrenaline)
Emergency drug for asthma
Isoproterenol HCL (Isoptel)
E. Norepinephrine (Levophed)
2. Inotropic / Cardiotonic Drugs
Milrinone (Primacor)
3. Intra Aortic Balloon Pump – to increase Carbon Dioxide by counter causation
Catheter is inserted via Femoral
4. If the 3 interventions failed: Prepare the Family for Death and Dying
Other Interventions
1. Maintain IV line
2. Drugs
Fibrinoytic Drugs= Dissolve clots
6- 12 hours
U – Urokinase
S - Streptokinase
A – Activase (Tissue Palsminogen Activase)
Side Effects: Bleeding
Antidote: Aminocaproic Acid
Anticoagulant = prevent thrombus formation; formation of new clots; extension or enlargement of clot

Antiplatelet = inhibits aggregation of platelet in the clotting process, decreases viscosity of the blood
A – Aspirin ( acethylsalysilic acid)
P – Plavix ( Clopidogrel)
P – Persantine (Dipherydamol) (no GI distress)
T – Ticlid (ticlopidiac HCL) (no GI distress)
Antilipidemic = lowers cholesterol in the blood
Bile Acid Sequestrant = Blocks bile; combines with bile to excrete in feces
Example: Cholestyramine (Questran) and Cholestipol (Colestid)
Side Effects: Constipation, Flatulence
B. HMG-Co A reductase Inhibitor = inhibits the formation of HMG- Primary State of building Cholesterol
Example:
R – Rosovostatin (Crestort)
A – Atorvastatin (Lipitor)
S – Simvastatin (Zocor)
Side Effects: Rhabdomyomyelysis ( muscle weakness)
Discontinue if blood lipids did not decrease within 3 months
3. EMOTIONAL SUPPORT
4. SEDATION – limit visitors, maintain quiet environment
5. TAKE TIME TO MAINTAIN ADEQUATE NUTRITION
NPO to decrease workload of the heart for 24 hours
Clear Liquids
Soft Diet after 48 hours
PRUDENT DIET: Low Salt, Low Fat, Low Cholesterol
6. PREVENT CONSTIPATION
Increase fiber and fluids if not contraindicated
Assist Exercise (Passive ROM)
7. ASSESS UNDERSTANDING OF SEXUALITY
4-6 weeks can resume for uncomplicated MI
Medications before sexual activity
Doctor’s clearance
Early morning foreplay
If 3 chest pain STOP then turn to side lying position
8. INSTRUCTION OF REHABILITATION
Maximum of 10 days
1 to 5 days ICU; CBR in 1-3 days on day 4-5 may sit (dangle the legs)
After 2 weeks follow-up care
NOTES ON COMPLICATIONS
1. CARDIAC TAMPONADE = accumulation of fluid/blood in the pericardial cavity (20-50ml) N=5-20 ml - Restrict ventricular filling
Hallmark Sign:
Pulsus Paradoxus (Decreased BP during INSPIRATION)
Jugular Vein Distention
Distant muffled heart sound
Intervention: PERICARDIOCENTESIS
The needle will be inserted in the pericardium; Semi-fowlers thru the xiphoid process
E-CART in place during cardiac arrest
2. DRESSLER’S SYNDROME = acute pericarditis that occur 2-3 weeks after MI attack
Hallmark Sign:
Chest pain- aggravated by coughing and breathing
Fever- pericarditis
Pericardial Friction Rub – scratchy/ high-pitched sound due to rubbing inflamed pericardial layers
Intervention:
Sitting on High-fowlers/Leaning forward
NSAID’s – Indomethacin
Anti-inflammatory – Steroids: Dexamethasone
3. ENDOCARDITIS = inflammation of the inner lining of the heart and heart valves
Etiology:
Dental abscess = most common cause
Drug users: fibrin
Vegetation (collection of bacteria, fibrin, RBC)
Hallmark Sign:
Low grade fever
Joint pain
Roth’s spot = retinal hemorrhage
Osler’s node = painful nodules on the pads of fingers and toes
Splinter’s hemorrhage = nail beds
Janeway’s Lesion = non-painful/non-tender hemorrhagic lesion at the sole of the foot
Intervention:
Bedrest = to prevent dislodgement of vegetation
Anti-embolic stocking
Monitor for signs of emboli
Blood Culture = determination of causative agent (Streptococcus/Staphylococcus)
NSAID’s
ATB : Penicillin G (cloxacillin/oxacillin)
Advise good oral hygiene 10-14 days to sterilize vegetations
Prophylaxis of ATB before any invasive procedures
II. CONGESTIVE HEART FAILURE
inability of the ventricles to pump normally
CARDIOMYOPATHY
Any disorder that affects the heart muscle is called a cardiomyopathy. Cardiomyopathy causes the heart to lose its ability to pump blood well. In some cases, the heart rhythm also becomes disturbed. This leads to arrhythmias (irregular heartbeats).
MANAGEMENT:
U – Upright position
N - Nitrates
L - Lasix
O - Oxygen
A - Aminophylline
D - Digoxin
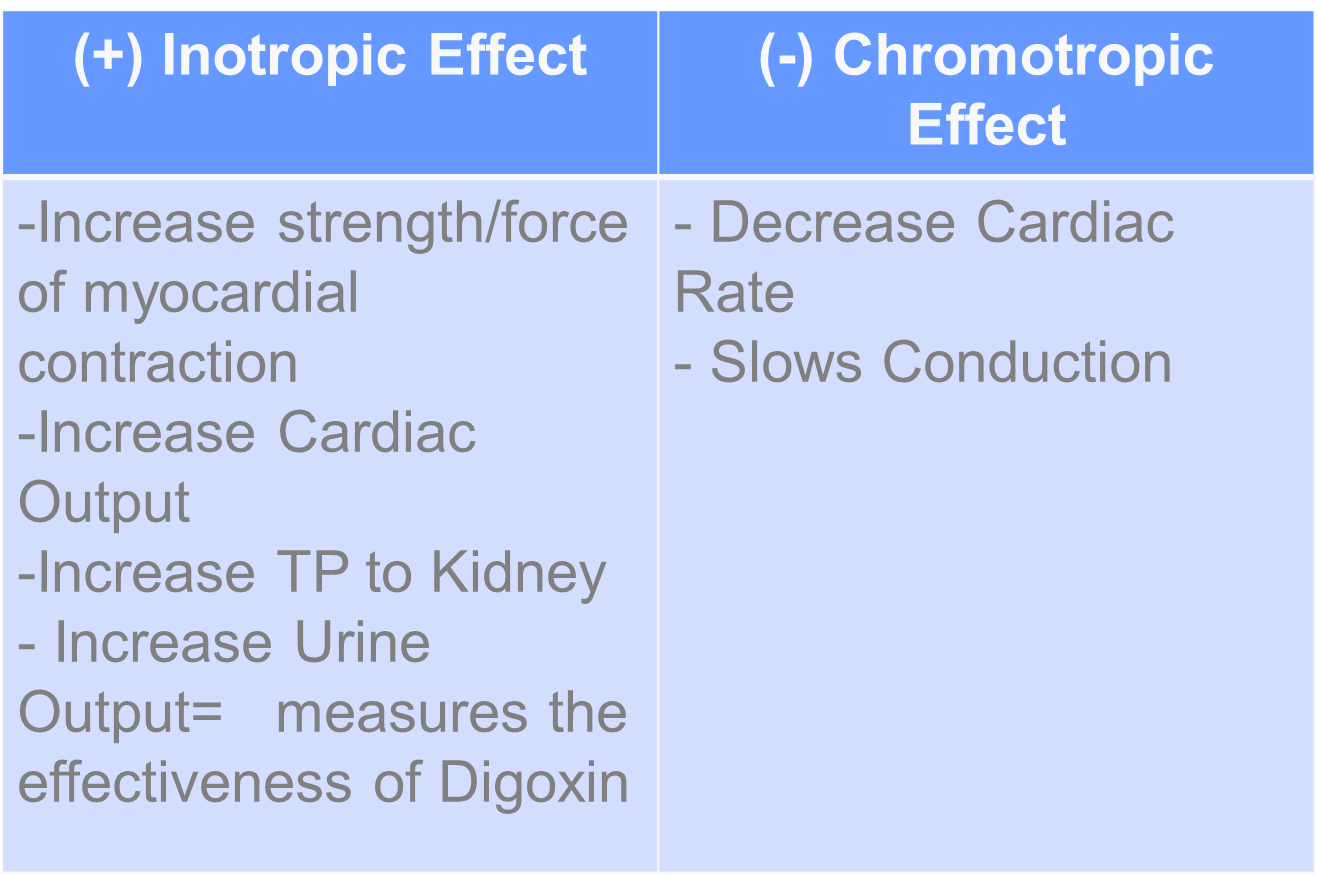
Digoxin Toxicity: GIT
V – Vomitus
A – Anorexia
N – Nausea
D – Diarrhea
A – Abdominal Pain
Therapeutic Level: 0.5-2 mg/dl
Antidote: Digibind or Ca EDTA
Withdraw blood before giving the drug or 8 hours after drug administration
F – Fluid Decrease
A – Afterload Decrease
ACE Inhibitor (Captopril)
Beta Blockers (olol)
S – Sodium Restriction
T – Test for Electrolytes (K level) Avoid Hypokalemia
Evident of U wave
Hypoactive Bowel Sounds
Weakness
D – Dry Phlebotomy – 3 extremities occluded, rotate every 15 minutes
III. ARRYTHMIAS
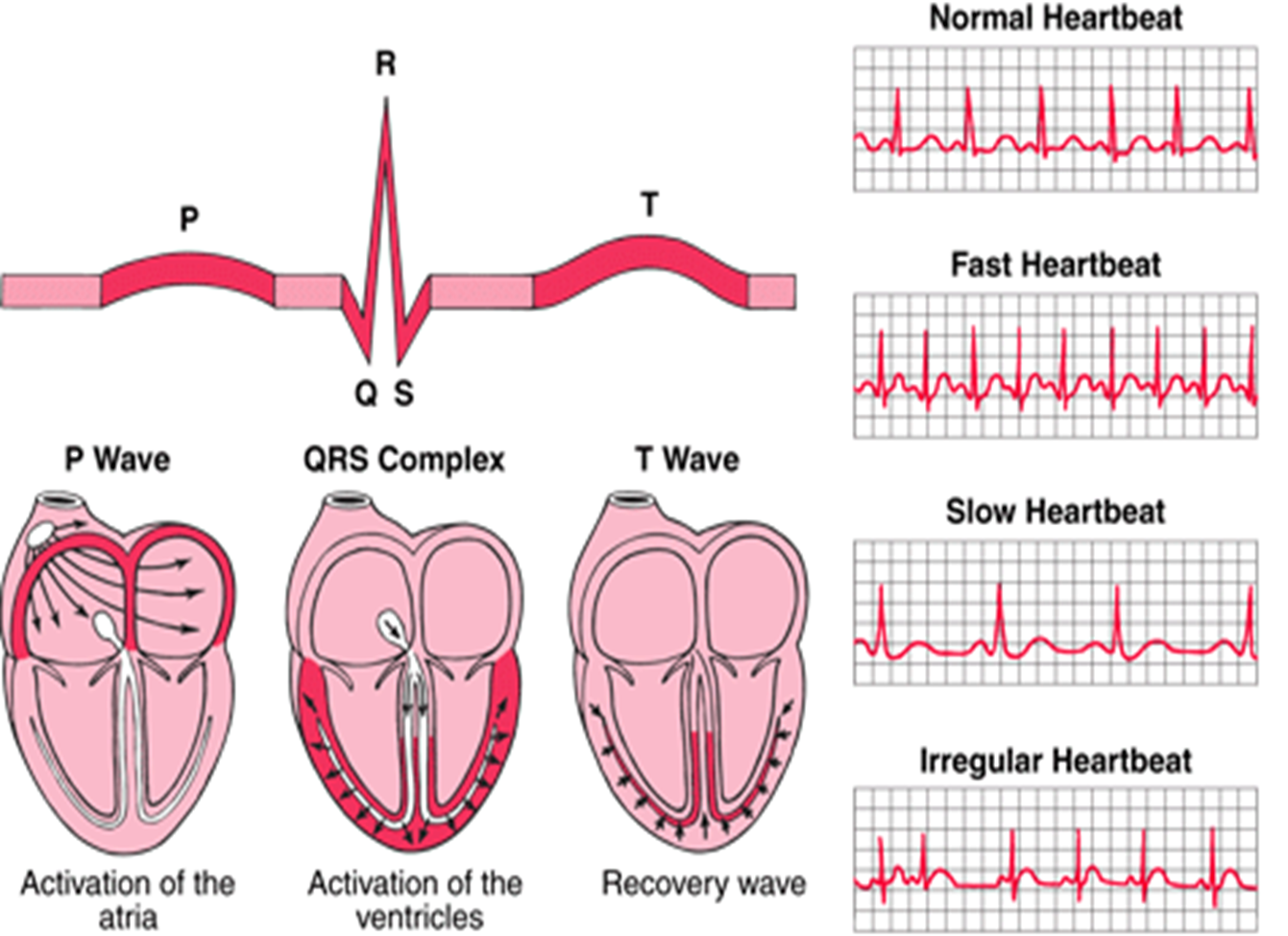
BRADYARRYTHMIAS
heart blocks; delayed transmission of impulse
1st AV-Block
Prolonged PR Interval
SA to AV
XXX to XXX
Asymptomatic
Do nothing because it is asymptomatic
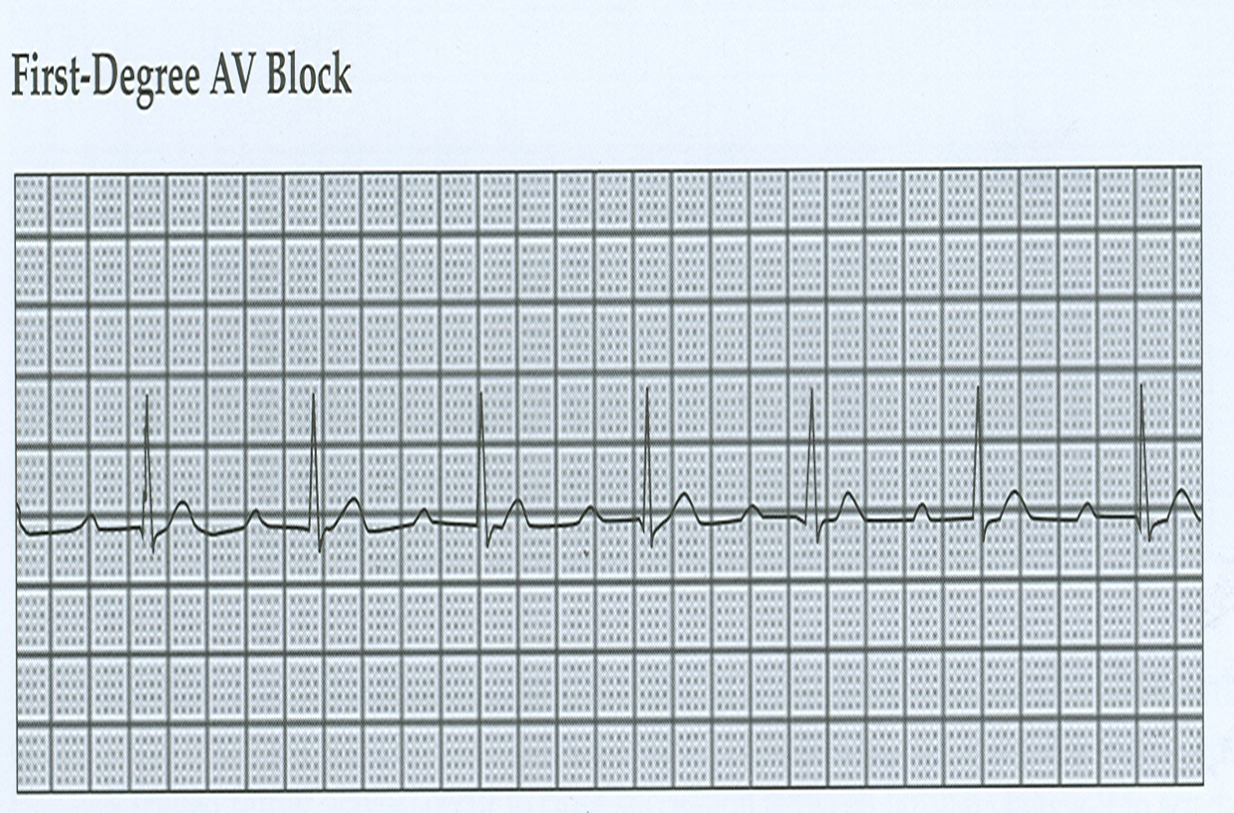
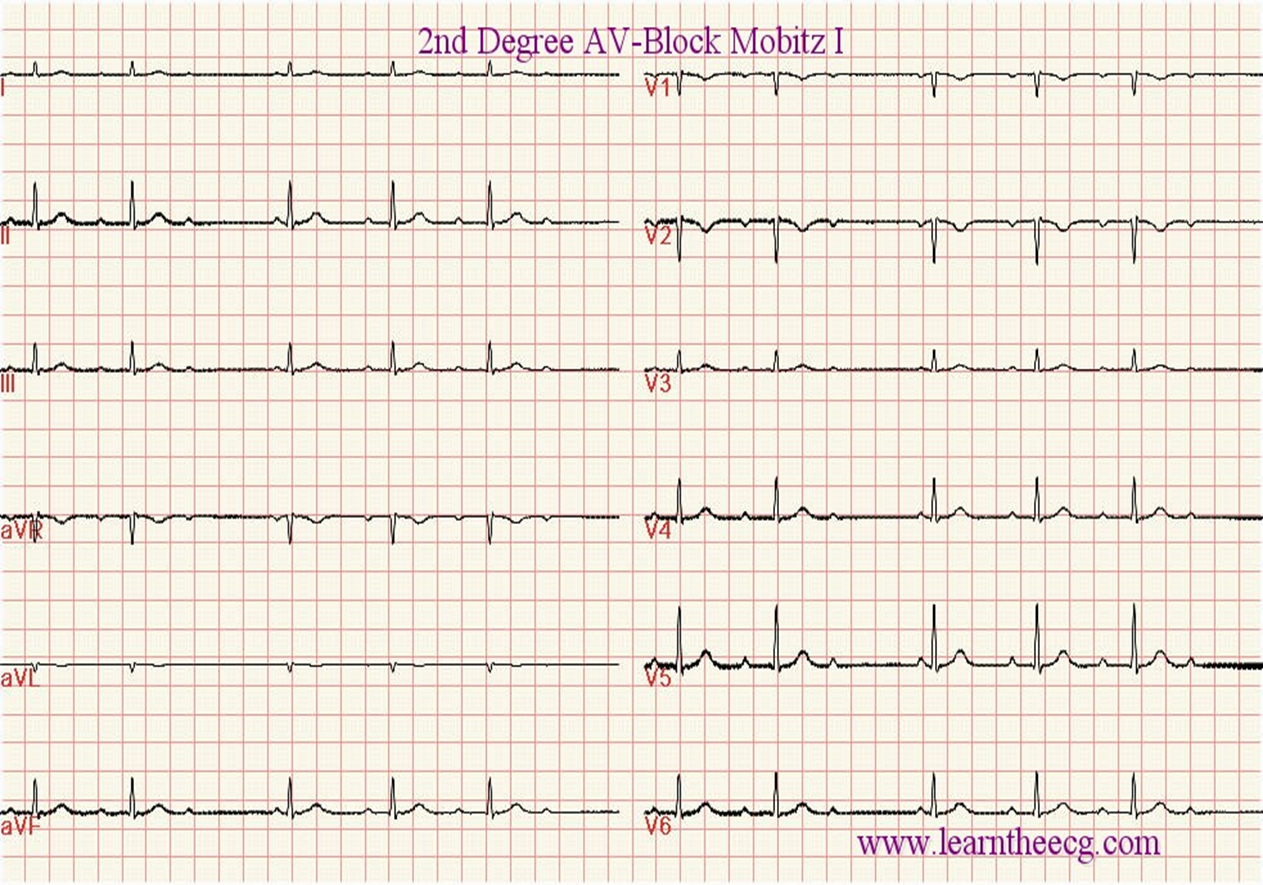
2nd AV-Block
MOBITS I – WEN KEBACHS - Progressive prolonged Interval
MOBITS II – Fixed prolonged interval
SA to AV
XXX to XX
Alteration in the patient’s level of conscious
Atropine Sulfate
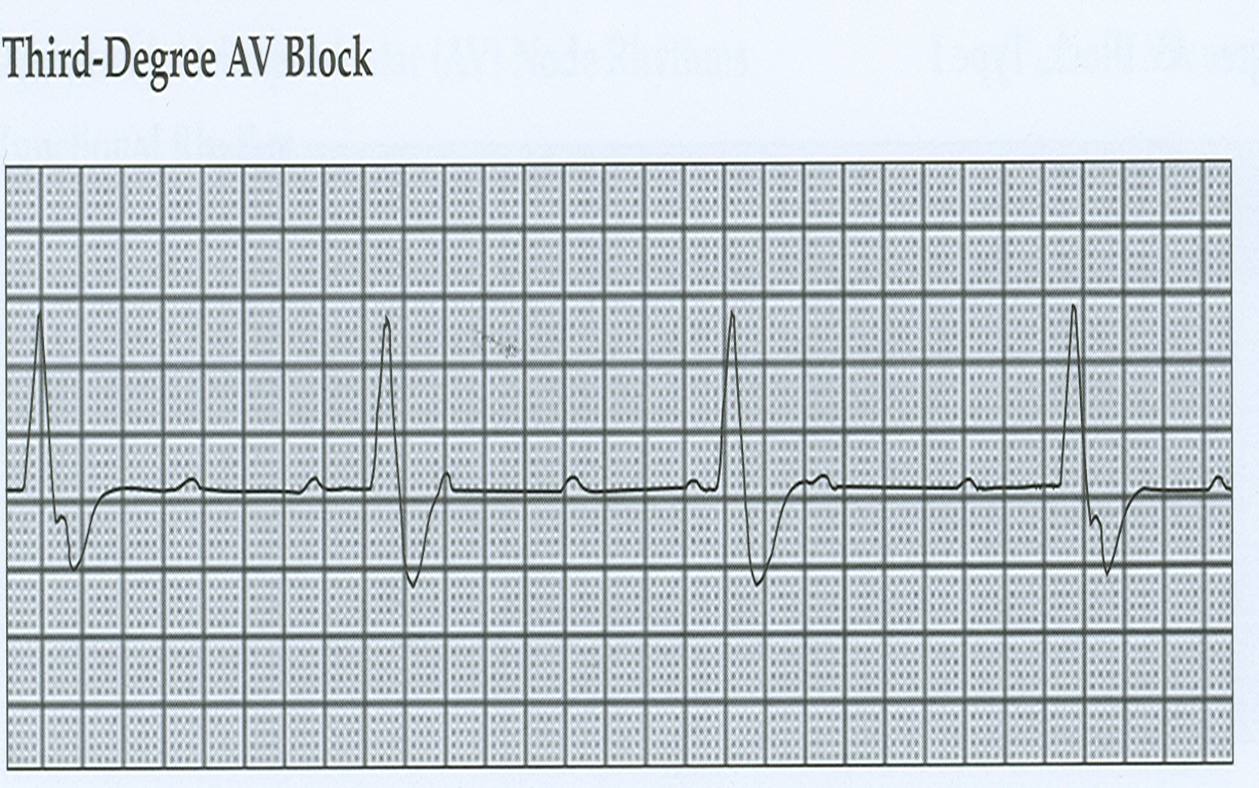
3rd AV-Block
Complete Block
SA to AV
XXX (No Impulse)
Treatment: Pacemaker
Types of Pacemakers:
Fixed/ Asynchronous = 4 beats/min = Notify
Present Cardiac Rate
Demand/Synchronous = Physiologic Demand
NURSING CONSIDERATIONS:
1. Take the patient’s pulse daily
2. No Contact sports/ wear loose fitting clothes
3. Daily dressing to prevent infection
4. Avoid electromagnetic devices
5. Common Pacemaker problems:
HICCUPS - 1st sign of PM malfunction
Failure to pace = fail to initiate impulse
Mx: Check the battery and placement of electrode
Failure to capture = regenerates impulse with no depolarization (tip of the catheter does not touch the heart)
Mx: Put the patient in Left Side-lying position
Failure to sense = does not sense cardiac rhythm and initiates an electrical impulse
Mx: Check the battery
6. Advise to keep pacemaker ID card in the wallet and wear
Medic-Alert Bracelet
TACHYARRYTHMIAS
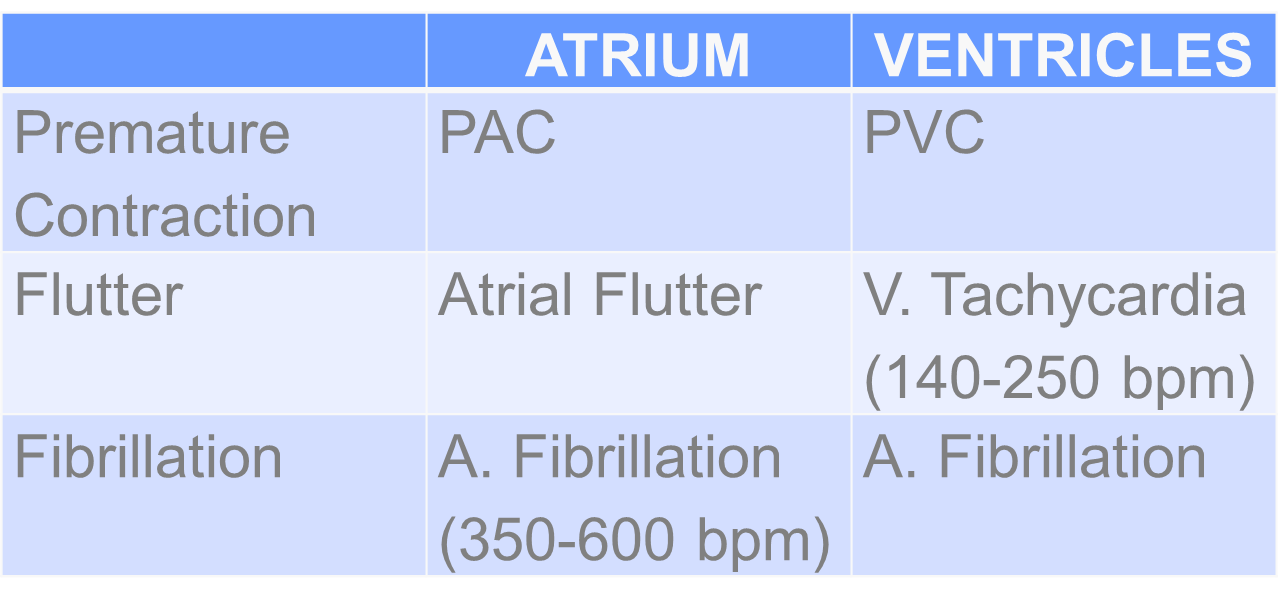
MANAGEMENT
Vagal Maneuver = induced vagal stimulation
Carotid Massage= 6-8 seconds
Valsalva Maneuver= Induces straining (Bear Down)
Induced Gag Reflex
Chemical Cardioversion
Quinidine (Quinine)
Procainamide- adverse reaction= SLE
Amniodarone (Cornderone)
Electrical Cardioversion
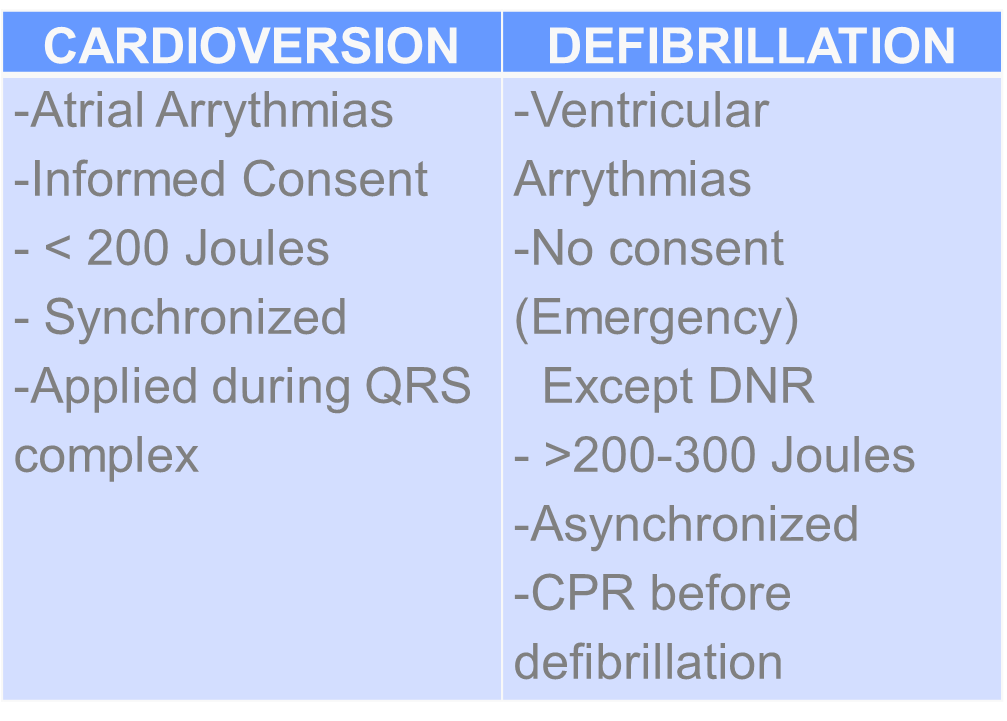
ATRIAL FIBRILLATION
Cardiac Arrhythmias
Cardiac Output Decreased
Cold Leg
Clot Formation
Treatment
Calan (Verapamil)
Calci Bloc
Cardizem
NURSING CONSIDERATIONS
Stop Oxygen during the procedure to avoid fire
Make sure to apply lubricant on paddles to avoid burns
Stay away from the bed when doctor say CLEAR
IV. VALVULAR HEART DISEASE
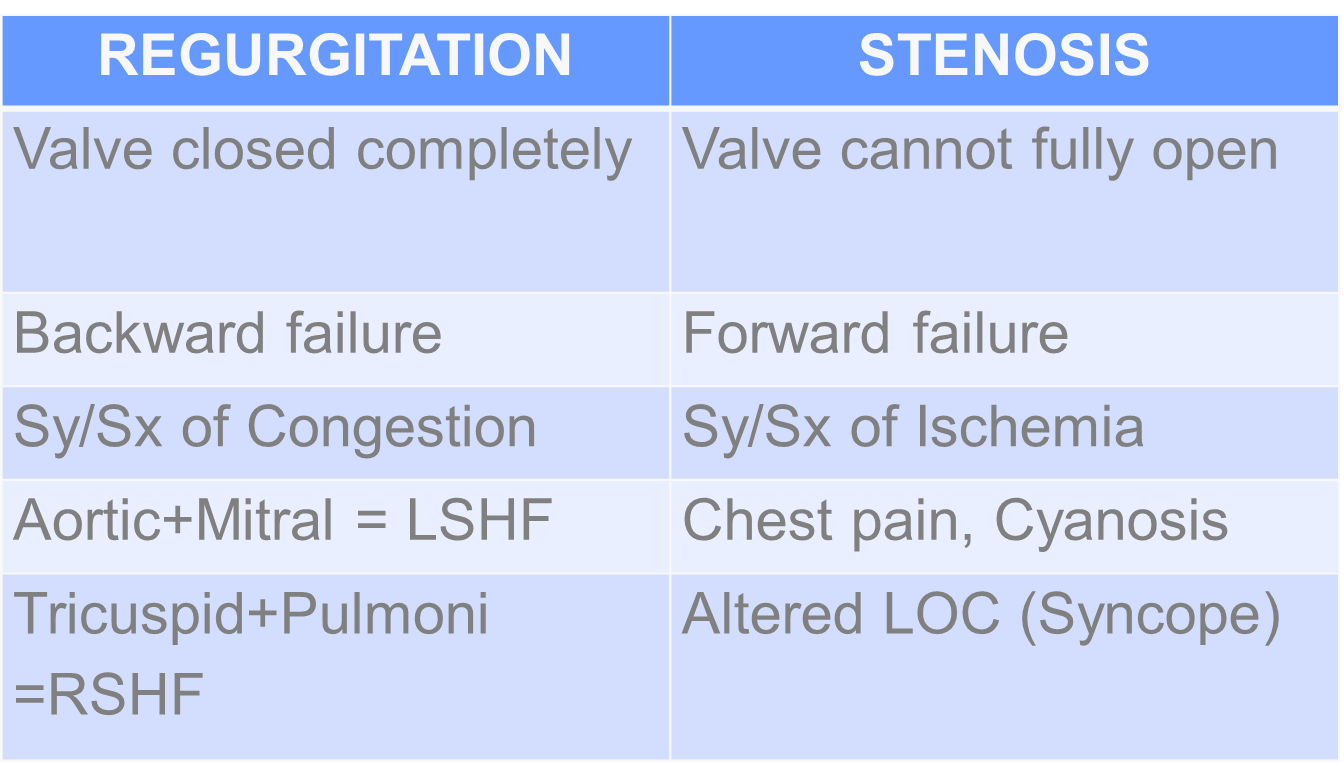
Diagnostic Test: Echocardiogram
Treatment: Only Surgical
Valvuloplasty - surgical repair of valve
Valvulotomy
V. PERIPHERAL VASCULAR DISEASE
Positioning
ARTERIAL: Flat on Bed
VENOUS: Elevated
Patency of the vessel
1. ATHEROSCLEROSIS OBLITERANS (ASO)
Chronic inflammation of vessels due to atheroma
2. THROMBOANGINITIS OBLITERANS (TAO)
Buerger’s Disease
Common: Men
Trigerred by: Smoking
BV = small and medium sized arteries of hands and feet
Hallmark Signs ( 6 P’s)
Paresthesia (Earliest)
Pain
Pallor
Paralysis
Poikilothermia
Pulselessness
Diagnostic Test:
Ankle Brachial Index
Formula: Ankle Pressure/Arm Pressure
110/70 / 120/80
40/40 = 1
Interpretation: If >.90 = Normal
0.71-0.90 = Mild
0.41-0.70 = Moderate
0.00-0.40 = Severe
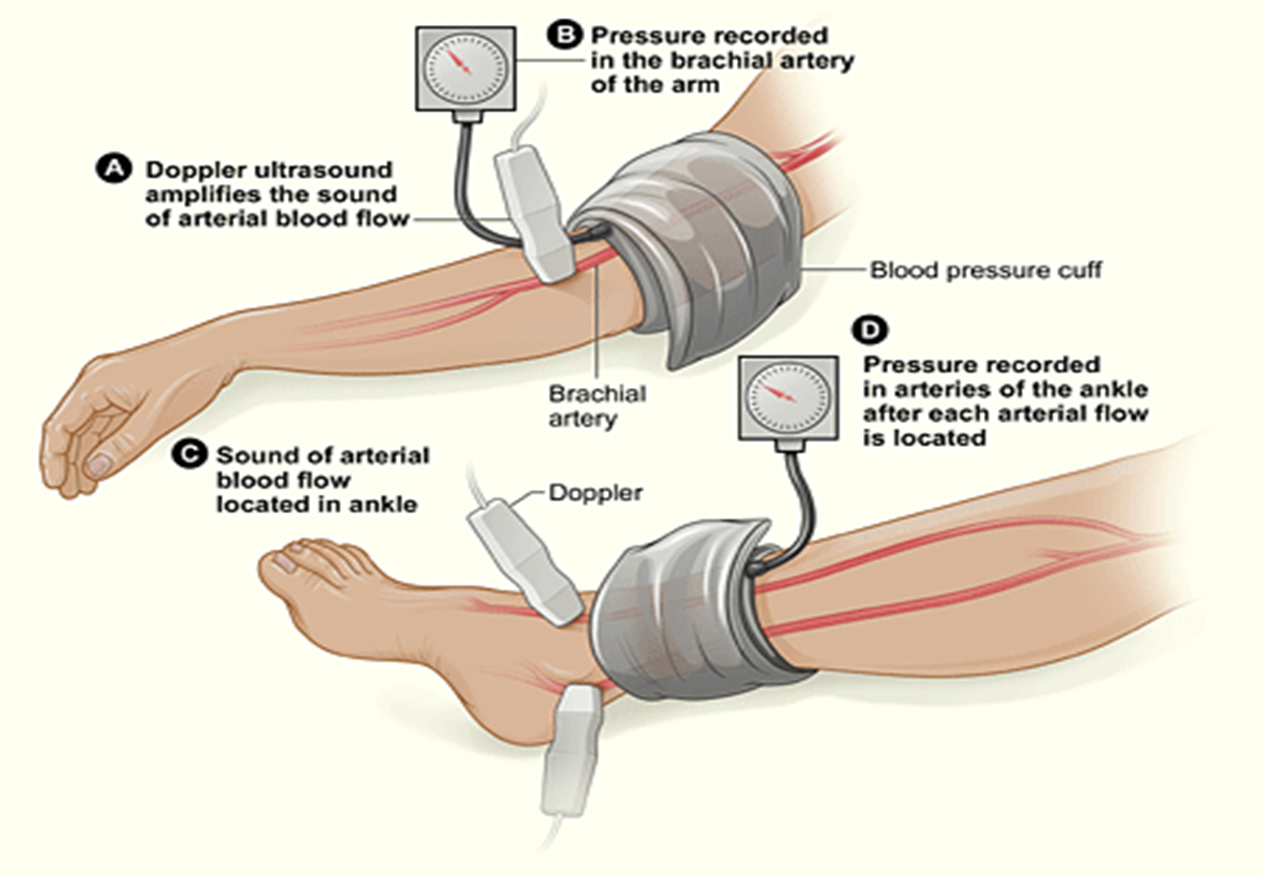
Doppler UTZ= monitor BV based on turbulence
Arteriography – Most reliable
MANAGEMENT
P – Promote adequate tissue perfussion
U – Understand Medications
Pentoxifylline
Papavarine
Plasma Expanders (Dextran)
Anticoagulant
Platelet Inhibitor
Antithrombotic (Cilostazol)
L – Limit/Stop Smoking and Caffeine
S – Safety of the leg = heat sensitive
No warm compress on the leg
Place it on the abdomen
Insulated leather shoes
E – Exercise: Buerger-Allen’s Exercise
Elevate extremities 5 degrees
Dangle the legs
Flat on bed
S – Surgery
Femoral-popliteal bypass graft
Rotational Atherectomy
Amputation
Pre-Op:
Psychological Preparation
Teach to prevent deformity
Phantom limb sensation
Post-Op:
Monitor for bleeding (always have a tourniquet)
No pillow under the knee (can cause flexion deformity)
Passive ROM
Prepare for crutchwalking
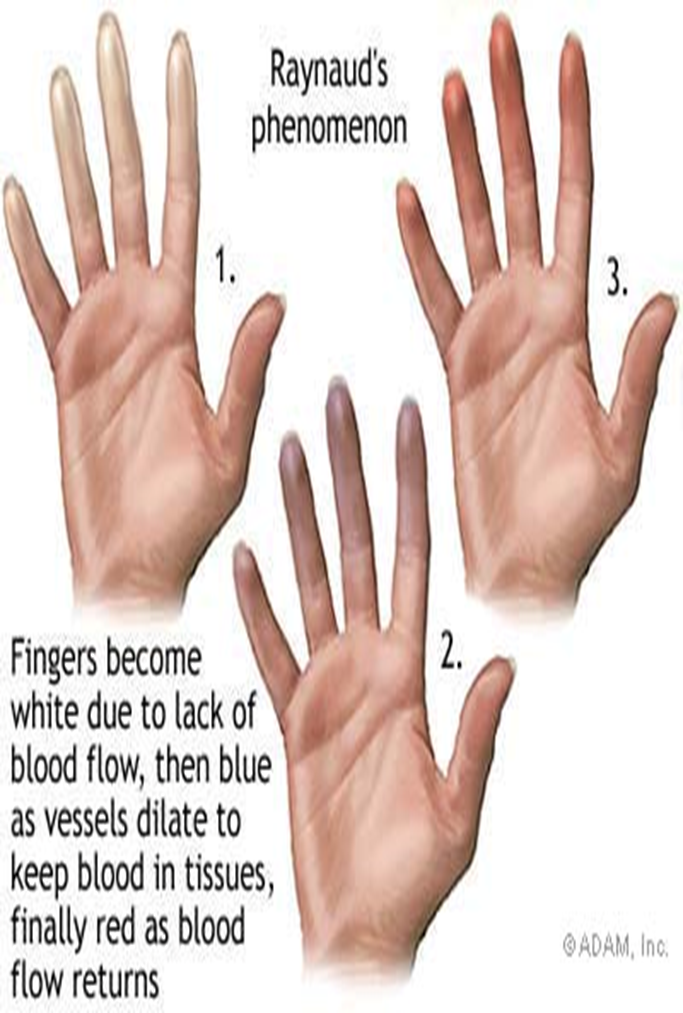
3. RAYNAUD’s PHENOMENON
– unknown etiology
Common : Female
Trigerred by : Smoking, Stress, Cold environment
Hallmark Sign: Flat color changes sign
Pallor = Whole - Vasoconstriction
Cyanotic = Blue - Vasoconstriction
Erythema = Red - Vasodilation
Diagnostic Test: Allen’s Test
Management
Reduce stress
Avoid cold environment
Use gloves and mittens
Use brandy/whisky (black label, red label)
Monitor pulse
Administer vasodilator
4. VENOUS DISORDERS (DVT)
PATENCY OF THE VESSELS
A. Inflammatory: Thrombophlebitis
Etiology
Hypercoagability of the blood
Endothelial Injury – blood vessel wall damage
Venous/Blood stasis- decrease venous return
Signs and Symptoms
Homan’s Sign
Increase in leg girth
Erythema of the leg
Edema
Management
Bedrest
Don’t massage(leg)
Elevate
Apply warm compress
Use elastic support
Improve hydration
Anti-coagulants
B. Functional: Varicose Vein
– abnormal dilation of vessel wall of vein
Etiology
Congenital, genetically weak BV
Prolonges sitting and standing
Signs and Symptoms
Dilated Tortorous vein
Dull achy sensation of the leg at the end of the day
Management
Elevate the leg
Foot massage
Note color changes
Hose applications
Ulcer treatment:
Stasis Dermatitis = non-healing ulcer of the leg
UNNA PASTE BOOT = dressing with zinc oxide to facilitate wound healing
Vein Stripping = veins larger for 4 months
Sclerotherapy = injection of solution to hardened vessels (2 -3 weeks)
Incision and Drainage
Pressure dressing for 12-18 hours
C. DEGENERATIVE: ANEURYSM
out patching of the artery due to damage in tunica media (congenitally weak)
Etiology:
S - Syphilis
A - Artherosclerosis (70%) enhanced by HTN
M - Marfan Syndrome
S – Sacular (one-sided dilated)
F – Fusiform ( 2 sided dilated)
D – Disecting (more sided dilated)
A – Abdominal
A – Aortic
A – Aneurysm
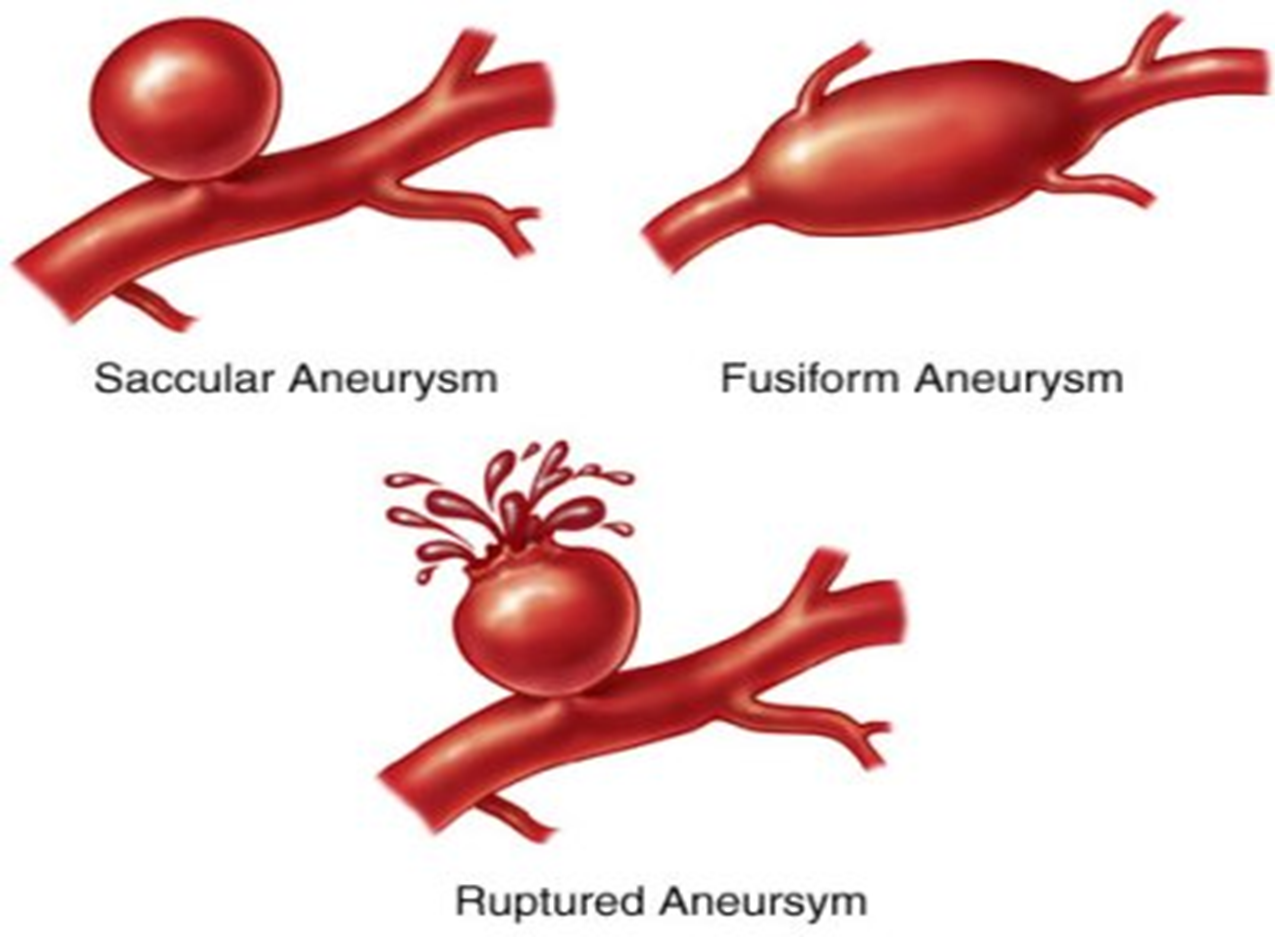
Consideration:
Do not palpate the abdomen = it can rupture
Asymptomatic
Abdominal mass pulsation
Flank pain/ Abdominal Pain (sign of aneurysm)
Sudden sharp knifelike pain (ruptured aneurysm)
D. CONSTRICTIVE: HYPERTENSION
TYPES
Primary = BP grading of 140/90 mmHg in 2 consecutive readings with 4-6 hours apart, unknown cause
Secondary = Secondary to disease
Ex. Chronic Renal Failure
Isolated = Calcification of Aorta R/T aging process
Seen in elderly
Asymptomatic
Most dangerous because it is related to high incidence of stroke
Malignant = Occipital headache due to anatomical placement of brain stem
Epistaxis
Paresthesia
Occipital Headache
MANAGEMENT
1. Lifestyle Modification
Diet: Prudent diet
Low alcohol
Stop smoking
2. Pharmacologic approach
A – ACE INHIBITORS “PRIL”
Vasoconstrictor
Side Effects: Bradycardia, HOPN, Pruritus, Cough, Angioedema
Nursing Considerations
Monitor the action of the drug
Contraindications
Patients with Renal Insufficiency
B – BETA BLOCKERS “OLOL”
B1 = Heart
Increase in Cardiac Rate, Increase BP
B2 = Lungs
Bronchodilation
P – Propranolol (Inderal)
A – Atenolol
T – Timolol
Contraindications: CHF/COPD
M – Metoprolol (Lopressor)
N – Nadolol (Corgard)
Blocks B1 can be given to asthmatic patients
C – CALCIUM – CHANNEL BLOCKERS
(-) INOTROPIC EFFECT = blocks the entrance of Calcium in the myocardial cell
Decreases Cardiac Contraction
C – Calan (Verapamil)
C – Cardizem
C – Calcibloc
A – Amlodipine (Norvasc)
N – Nifedipine (Procardia)
Contraindications: CHF
D – DIURETICS
A – Aldactone (Spinorolactone) K Sparring
Side Effects: Hyperkalemia = Irregular heartbeats
B – Bumex = Ototoxicity
C – Chlorthiazide ( Diuril) = K wasting; can cause Pancreatitis- monitor Amylase
F – Furosemide (Lasix) = Loop Diuretic